-
Reagents
- Flow Cytometry Reagents
-
Western Blotting and Molecular Reagents
- Immunoassay Reagents
-
Single-Cell Multiomics Reagents
- BD OMICS-Guard™ Sample Preservation Buffer
- BD® AbSeq Assay
- BD® Single-Cell Multiplexing Kit
- BD Rhapsody™ ATAC-Seq Assays
- BD Rhapsody™ Whole Transcriptome Analysis (WTA) Amplification Kit
- BD Rhapsody™ TCR/BCR Next Multiomic Assays
- BD Rhapsody™ Targeted mRNA Kits
- BD Rhapsody™ Accessory Kits
- BD® OMICS-One Protein Panels
- BD OMICS-One™ WTA Next Assay
-
Functional Assays
-
Microscopy and Imaging Reagents
-
Cell Preparation and Separation Reagents
Old Browser
This page has been recently translated and is available in French now.
Looks like you're visiting us from {countryName}.
Would you like to stay on the current location site or be switched to your location?

Allergies
Allergy is an overactive immune (hypersensitivity) reaction to a harmless entity sensed as dangerous by the immune system. Type 1 hypersensitivity involves the production of Ig-E antibodies against an allergen. Different types of allergies have been described and include food allergies, drug allergies, allergies to plant components (pollen) and allergies to animal products. Manifestations of allergic reactions include redness of the skin (contact allergy), sneezing, wheezing and edema and can ultimately lead to anaphylactic shock. Different populations of immune cells are engaged in an allergic reaction, including antigen presenting cells (e.g., dendritic cells), mast cells and Ig-E producing B cells and T cells.
What causes allergy?
Most allergies are caused by a known allergen but cases of allergies of unknown origin exist. Allergens can be airborne (e.g., pollen, dust) or can come from the food ingested (e.g., peanut, eggs, shellfish), medications consumed or substances that come into contact with the skin (e.g., latex, insect bite).
Different Types of Hypersensitivity
Type I hypersensitivity: anaphylactic response
Type I hypersensitivity reaction, also known as anaphylactic response, is characterized by a rapid Ig-E antibody production. These Ig-E bind to mast cells and basophils and induce the release of histamine-containing granules. Some examples of type I hypersensitivity reactions include food allergy, allergic rhinitis, allergic bronchial asthma, atopic eczema, drug allergy and anaphylactic shock.1

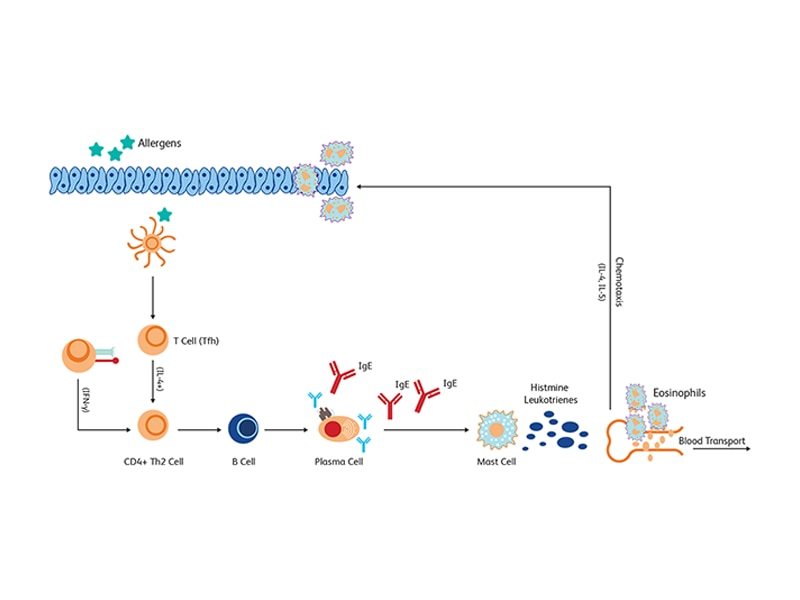
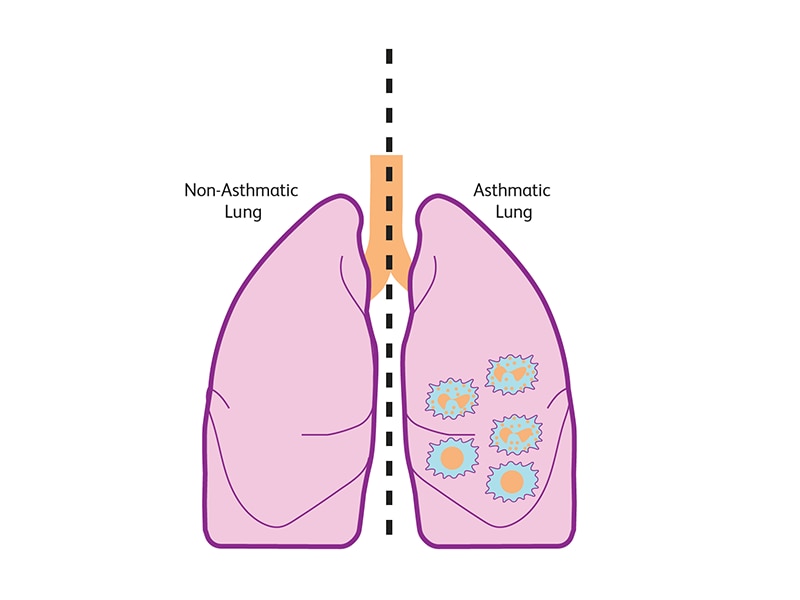
In type 1 asthma, the Ig-E bind to mast cells, resulting in the release of histamines and leukotrienes leading to inflammation of eosinophils, which is a hallmark of allergic inflammatory response and a degranulation process. This is also accompanied by the release of inflammatory cytokines such as IL-4 and IL-5.2
Type II hypersensitivity: cytotoxic
Type II hypersensitivity is characterized by Ig-M and Ig-G antibodies that bind to cell surface antigens inducing activation of complement cascades and phagocytosis.1 Type II hypersensitivity reactions are common in some types of autoimmune diseases, such as autoimmune neutropenia of rheumatoid disorders.

Type III hypersensitivity: immune complex reaction
Type III hypersensitivity reaction is also known as immune-complex reaction. It also involves Ig-M and Ig-G antibodies, but they react with soluble antigens. The complement system is also activated, and chemo-attracted neutrophils cause local inflammation and tissue damage. This type of hypersensitivity is observed in serum sickness arthritis and glomerulonephritis. Other types of antibodies such as Ig-A have also been described in type III hypersensitivity. In Berger’s disease, also known as immunoglobulin A nephropathy, damage of the kidney is linked to Ig-A deposits and local inflammation.3

Type IV hypersensitivity: delayed reaction
A fourth type of hypersensitivity is classified as delayed hypersensitivity reaction (DHR) and is characterized by infiltration of antigen-specific T cells. Different subtypes of type IV hypersensitivity are described based on the infiltrating T cells: type IV-a, -b, -c, -d associated with Th1, Th2, T-effector and GM-CSF producing T cells, respectively.4

References
- Justiz Vaillant AA, Vashisht R, Zito PM. Immediate hypersensitivity reactions. In: StatPearls. Treasure Island (FL): StatPearls Publishing; August 16, 2020.
- Peebles RS, Jr, Aronica MA. Proinflammatory pathways in the pathogenesis of asthma. Clin Chest Med. 2019;40(1):29-50. doi:10.1016/j.ccm.2018.10.014
- Stanley JC, Deng H. Progress in pathogenesis of immunoglobin A nephropathy. Cureus. 2020;12(6):e8789. doi:10.7759/cureus.8789
- Meng X, Yerly D, Naisbitt DJ. Mechanisms leading to T-cell activation in drug hypersensitivity. Curr Opin Allergy Clin Immunol. 2018;18(4):317-324. doi:10.1097/ACI.0000000000000458
Common types of allergy
Food allergy and oral tolerance
Food allergies can be subdivided into three main categories based on the extent of involvement of Ig-E.1
Ig-E-mediated food allergy
Ig-E-mediated food allergy involves the binding of food allergens to Ig-E molecules leading to the activation of effector cells releasing histamine (immediate response) followed by allergic inflammation with increased leukotrienes, platelet activating factor (PAF), and IL-4, IL-5 and IL-13 cytokines.1
Non-Ig-E mediated food allergy
Non-Ig-E mediated food allergies mostly affect the gastrointestinal tract. In food protein–induced ailments such as food protein–induced enterocolitis syndrome (FPIES), food protein–induced proctocolitis (FPIP) and food protein enteropathy (FPE), allergen-specific T cells have been described.1 Cutaneous exposure to food allergens has been shown to promote sensitization and TH2 mediated responses in the gut. Retinoic acid secreted by antigen presenting cells can induce the expression of gut homing receptors in T cells but also Ig-A secreting B cells and provoke their migration to the gut.1,2 Exposure to dietary gluten causes celiac disease, a T-cell-mediated autoimmune disorder in individuals predisposed to autoimmune diseases.3
Mixed food allergy
Mixed food allergy involves Ig-E dependent and Ig-E independent pathways. Some examples include atomic dermatitis and eosinophilic gastrointestinal disorders (e.g., eosinophilic esophagitis). In this type of reaction, a distinct Th-2 response profile (eotaxin‐3, IL‐5, IL‐5 receptor α‐chain and IL‐13) along with tissue infiltration by inflammatory eosinophils and elevated levels of IL‐1α, IL‐6 and IL‐8 in the peripheral blood are observed.1,4
Drug allergy
Adverse drug reactions (ADR) are divided into two types: type A and type B. Type A ADR is a predictable reaction related to the dosing of a drug. Type B ADR is unpredictable and not related to the drug dose and the response closely resemble an allergic reaction.5 Antibiotics allergy and vaccine hypersensitivity are two examples of drug allergies. These reactions can be Ig-E or non-Ig-E mediated.
Antibiotics allergy
In some antibiotic allergies (e.g., angioedema, urticarial) Ig-E mediated reactions are induced after binding of antibiotics allergens to Ig-E expressed on mast cells and basophils. In other allergies such as those induced by vancomycin and fluoroquinolones, mast-cell and basophils are activated and non-IgE-mediated reactions are elicited but no immunological memory is formed.6,7
Vaccine hypersensitivity
Vaccine-associated hypersensitivity reactions can occur because of a reaction with a vaccine component (e.g., antigen of interest) or with a preservative or other microbial antigen (e.g., tetanus) used to potentiate vaccine-induced immune responses (e.g., aluminum adjuvant). Several types of hypersensitivity reactions have been described, including Ig-E, Ig-G, complement mediated responses as well as delayed T cell–mediated responses and rare cases of anaphylaxis (1.31 cases per million doses).8
References
- Yu W, Freeland DMH, Nadeau KC. Food allergy: immune mechanisms, diagnosis and immunotherapy. Nat Rev Immunol. 2016;16(12):751-765. doi:10.1038/nri.2016.111
- Hammerschmidt SI, Friedrichsen M, Boelter J, et al. Retinoic acid induces homing of protective T and B cells to the gut after subcutaneous immunization in mice. J Clin Invest. 2011;121(8):3051-3061. doi:10.1172/JCI44262
- Jabri B, Sollid LM. T cells in celiac disease. J Immunol. 2017;198(8):3005-3014. doi: 10.4049/jimmunol.1601693
- Simon D, Cianferoni A, Spergel JM, et al. Eosinophilic esophagitis is characterized by a non-IgE-mediated food hypersensitivity. Allergy. 2016;71(5):611-620. doi:10.1111/all.12846
- Park JS, Suh DI. Drug allergy in children: what should we know? Clin Exp Pediatr. 2020;63(6):203-210. doi:10.3345/kjp.2019.00675
- Blumenthal KG, Peter JG, Trubiano JA, Phillips EJ. Antibiotic allergy. Lancet. 2019;393(10167):183-198. doi:10.1016/S0140-6736(18)32218-9
- Chiriac AM, Banerji A, Gruchalla RS, et al. Controversies in drug allergy: drug allergy pathways. J Allergy Clin Immunol Pract. 2019;7(1):46-60.e4. doi:10.1016/j.jaip.2018.07.037<
- McNeil MM, DeStefano F. Vaccine-associated hypersensitivity. J Allergy Clin Immunol. 2018;141(2):463-472. doi:10.1016/j.jaci.2017.12.971
Assays for studying allergy-related immune responses
Serum cytokine detection
The BD® CBA Human Inflammatory Cytokines Kit can be used to quantitatively measure interleukin-8 (IL-8), interleukin-1β (IL-1β), interleukin-6 (IL-6), interleukin-10 (IL-10), tumor necrosis factor (TNF) and interleukin-12p70 (IL-12p70) protein levels in a single sample.
Measurement of complement activation
The BD® CBA Human Anaphylatoxin Kit can be used to quantitatively measure anaphylatoxin C3a, C4a and C5a (bioactive cleavage products released from C3, C4 and C5 during complement activation) protein levels in a single EDTA plasma or serum sample.
Mediator releasing cells phenotyping
The TX83 monoclonal antibody specifically recognizes Allergin-1, which is also known as Allergy inhibitory receptor 1 or Mast cell antigen 32 (Mast cell Ag-32/ Mca32). Allergin-1 is a ~60 kDa type I transmembrane glycoprotein that is encoded by Milr1 (Mast cell immunoglobulin like receptor 1) and contains two cytoplasmic immunoreceptor tyrosine-based inhibitory motifs. Allergin-1 is expressed on mast cells as well as some dendritic cells, macrophages and neutrophils. When ligated with FcεRI, Allergin-1 inhibits FcεRI-mediated degranulation of mast cells, which suppresses immediate hypersensitivity reactions.
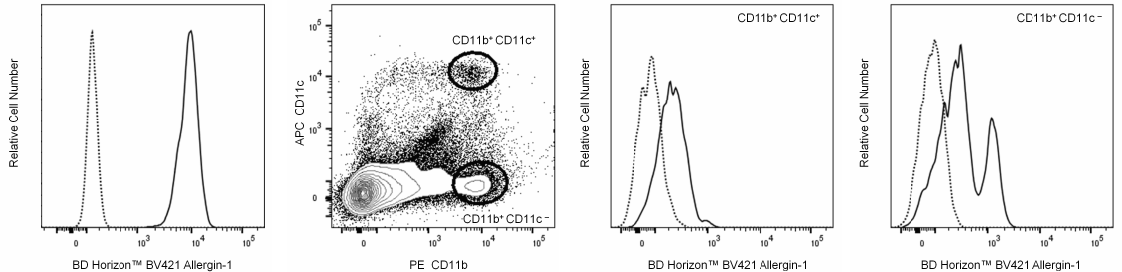
Flow cytometric analysis of Allergin-1 expression on mouse CD117+ (mast cells) peritoneal exudate cells (far left histogram). BALB/c peritoneal exudate cells (PECs) were stained with BD Pharmingen™ APC Rat Anti-Mouse CD117 Antibody (Cat. No. 553356/561074) and 1 μg/test of either BD Horizon Brilliant Violet™ 421 (BV421) Mouse IgG1, κ Isotype Control (Cat. No. 562438; dotted line histogram) or BD Horizon™ BV421 Mouse Anti-Mouse Allergin-1 Antibody (Cat. No. 566340; solid line histogram). The fluorescence histogram showing Allergin-1 expression (or Ig isotype control staining) was derived from CD117-positive events with the forward and side light-scattered characteristics of viable PECs. Flow cytometric analysis was performed using a BD FACSCanto™ II Flow Cytometer System. Data shown are not specific.
Multicolor flow cytometric analysis of Allergin-1 expression on mouse splenic leucocyte populations (middle left, middle right, far right). BALB/c mouse splenic leucocytes were stained with BD Pharmingen™ PE Rat Anti-Mouse CD11b (Cat. No. 553311/557397/561689) and BD Pharmingen™ APC Hamster Anti-Mouse CD11c (Cat. No. 550261/561119) Antibodies and 1.0 μg/test of either BD Horizon Brilliant Violet™ 421 (BV421) Mouse IgG1, κ Isotype Control (Cat. No. 562438; dotted line histograms) or BD Horizon™ BV421 Mouse Anti-Mouse Allergin-1 Antibody (Cat. No. 566340; solid line histograms). Histograms showing Allergin-1 expression (or Ig isotype control staining) were derived from CD11b+CD11c+ (dendritic cells) or CD11b+CD11c- (monocytes/macrophages) gated events with the forward and side light-scattered characteristics of viable leucocyte populations as indicated. Flow cytometric analysis was performed using a BD FACSCanto™ II Flow Cytometer System. Data shown are not lot specific.
Measuring mitochondrial function in allergy
Mitochondrial dysfunctions are observed in allergy, which include changes in mitochondrial membrane potential (MMP), transcription factor phosphorylation status (e.g., STAT3), and oxidative stress with increased reactive oxygen species (ROS) production.1,2 The mitochondrial membrane potential can be monitored with the BD® MitoScreen Kit. Stat3 phosphorylation on serine 727 is critical to mast cell degranulation and can be monitored using the BD Phosflow™ Alexa Fluor™ 488 Mouse Anti-Stat3 (pS727) Antibody.
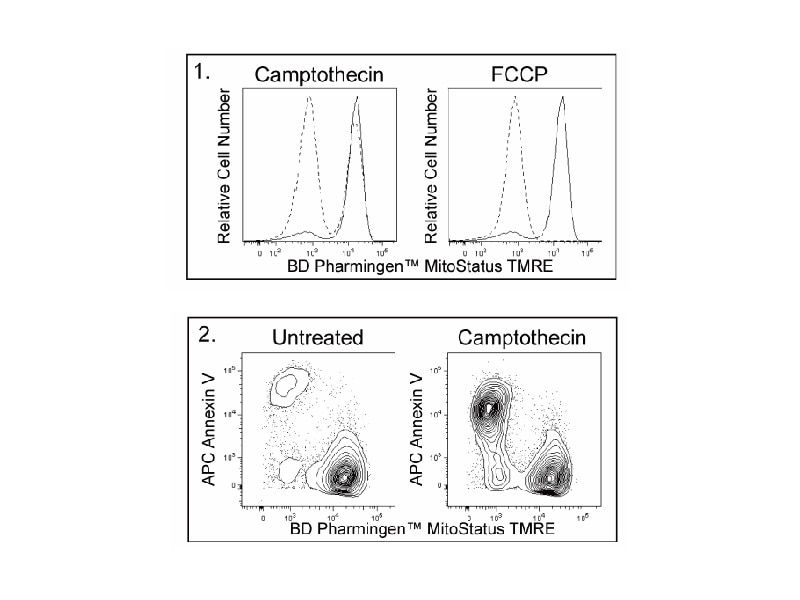
The BD Pharmingen™ MitoStatus TMRE (tetramethylrhodamine ethyl ester) is a fluorescent dye that is readily sequestered by active mitochondria, allowing for flow cytometric or imaging analysis to assess for apoptosis or mitochondrial depolarization. Cells with polarized mitochondria will fluoresce red while apoptotic or cells with depolarized mitochondria will have diminished levels of red fluorescence.
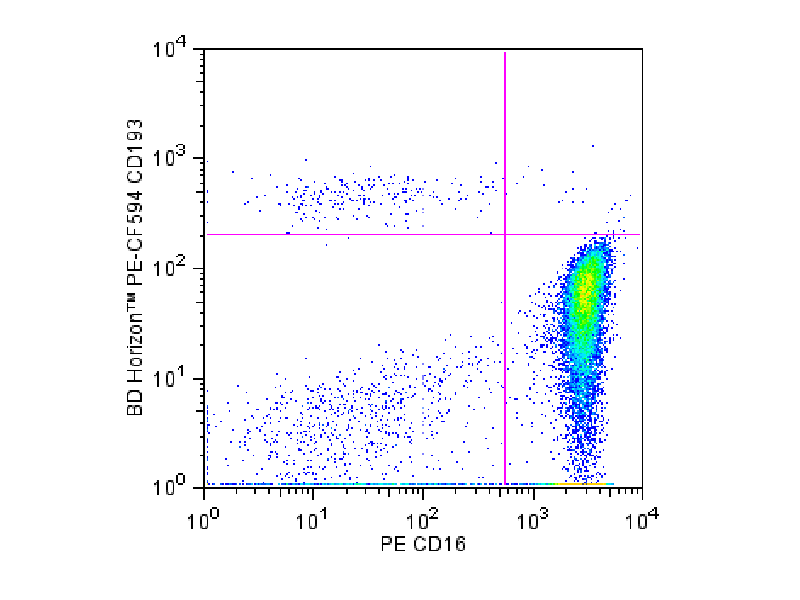
Flow cytometric analysis of CD193 expression on human peripheral blood granulocytes (eosinophils). Whole blood was stained with BD Horizon™ PE-CF594 Mouse Anti-Human CD193 Antibody (Cat. No. 562571) and PE Mouse Anti-Human CD16 Antibody (Cat. No. 555407/560995). The erythrocytes were lysed with BD Pharm Lyse™ Lysing Buffer (Cat. No. 555899). Two-color flow cytometric dot plots showing the correlated expression of CD193 versus CD16 was derived from events with the forward and side light-scatter characteristics of viable granulocytes. Flow cytometry was performed using a BD® LSR II Flow Cytometer System.
Immunophenotyping of atopy
CD193 or CCR3 is primarily expressed by eosinophils and basophils during atopic conditions, dermatitis, allergic rhinitis, conjunctivitis and bronchial asthma. BD Biosciences offers a variety of antibodies, such as BD OptiBuild™ CD193, BD Horizon™ CD193 and BD Pharmingen™ CD193 Antibodies, to detect CD193.
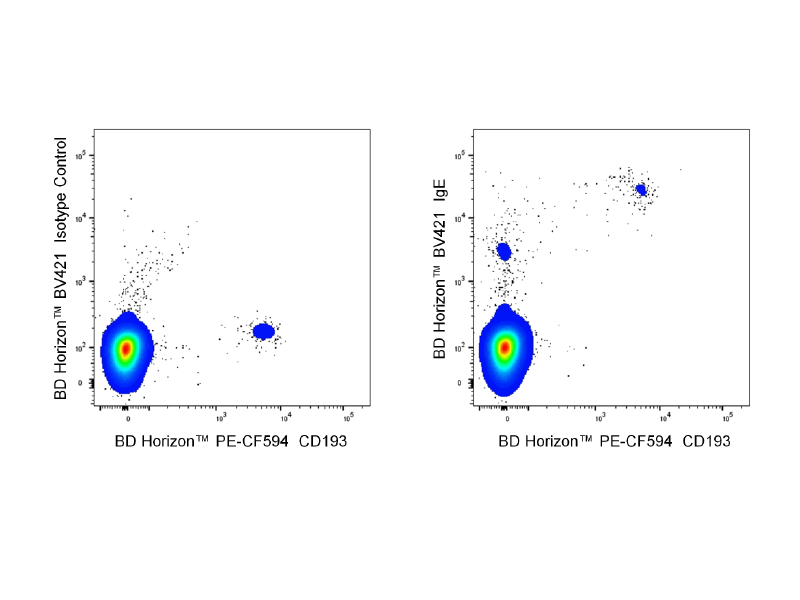
Monitoring Ig-E expression
Two-color flow cytometric analysis of IgE expression on human peripheral blood leucocytes. Whole blood cells were stained with BD Horizon™ PE-CF594 Mouse Anti-Human CD193 Antibody (Cat. No. 562571) and either BD Horizon Brilliant Violet™ 421 (BV421) Mouse IgG2a, κ Isotype Control (Cat. No. 562439; left plot) or BD Horizon™ BV421 Mouse Anti-Human IgE Antibody (Cat. No. 566324/566325; right plot). Erythrocytes were lysed with BD Pharm Lyse™ Lysing Buffer (Cat. No. 555899). The two-color flow cytometric dot plot showing the correlated expression of CD193 versus IgE (or Ig Isotype control staining) was derived from gated events with the forward and side light-scatter characteristics of viable lymphocytes. Flow cytometric analysis was performed using a BD LSRFortessa™ Cell Analyzer System.
References
- Qin S, Wang X, Wu H, et al. Cell-based phenotypic screening of mast cell degranulation unveils kinetic perturbations of agents targeting phosphorylation. Sci Rep. 2016;6:31320. doi:10.1038/srep31320
- Ramakrishnan RK, Bajbouj K, Al Heialy S, et al. IL-17 induced autophagy regulates mitochondrial dysfunction and fibrosis in severe asthmatic bronchial fibroblasts. Front Immunol. 2020;11:1002. doi:10.3389/fimmu.2020.01002
For Research Use Only. Not for use in diagnostic or therapeutic procedures.
Alexa Fluor is a trademark of Life Technologies Corporation. CF is a trademark of Biotium, Inc.